New study advocates remission as therapeutic goal in prediabetes
Prediabetes is a condition that precedes type 2 diabetes and increases the risk of heart attack, kidney and eye disease, and several types of cancer. There is no approved drug therapy for prediabetes available. Scientists at the German Center for Diabetes Research (DZD) now show how and by which mechanisms prediabetes can be brought into remission, i.e. into a state in which blood glucose levels return to normal. The study shows that this protects against type 2 diabetes and is associated with better kidney and vascular function in the long term. The underlying mechanisms are different from those in type 2 diabetes remission, the researchers report in The Lancet Diabetes & Endocrinology.
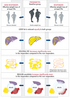
People with type 2 diabetes have an increased risk of heart attack, kidney disease, and stroke, and a higher mortality risk. Type 2 diabetes was thought to be irreversible until a few years ago. We now know that type 2 diabetes can be put into remission in a significant number of individuals through substantial weight loss. However, this remission rarely lasts as most people typically develop type 2 diabetes again within a few years.
"We aimed to explore the feasibility of commencing earlier and implementing preventive measures already at a stage that precedes type 2 diabetes, namely prediabetes, with the aim of reversing it," elucidates senior author Prof. Dr. Andreas Birkenfeld, Medical Director of Medical Clinic IV at Tübingen University Hospital, and Director of the Institute for Diabetes Research and Metabolic Diseases of Helmholtz Munich at the University of Tübingen. This could be crucial for patients with prediabetes as they are at increased risk of developing type 2 diabetes as well as heart, kidney, and eye complications among others.
But what causes prediabetes to go into remission? Scientists from the Institute of Diabetes Research and Metabolic Diseases (IDM) at Helmholtz Munich and the Department of Diabetology, Endocrinology, and Nephrology at the University Hospital of Tübingen, conducted a post-hoc analysis on participants with prediabetes from the Prediabetes Lifestyle Intervention Study (PLIS) to investigate this question.
In this randomized-controlled multicenter study conducted by the DZD, 1,105 individuals with prediabetes underwent a lifestyle intervention involving a healthy diet and increased physical activity for a duration of one year. The researchers then assessed the 298 participants who had achieved a minimum weight loss of five percent as a result of the intervention. Responders were the participants whose fasting blood glucose, 2-hour glucose, and HbA1c levels had normalized within twelve months, indicating that they had gone into remission. Non-responders were individuals who did not achieve remission despite losing weight and still had prediabetes.
Contrary to the researchers' initial assumptions, it was not weight loss that distinguished those who went into remission from those who did not, as there was no difference in relative weight loss between responders and non-responders. However, individuals who achieved remission demonstrated a notable improvement in insulin sensitivity compared to non-responders. In essence, they were able to enhance their sensitivity to insulin, a hormone that lowers blood glucose levels, significantly more than those who did not respond. Nonetheless, the quantity of insulin secreted remained unaltered in both groups. This difference is critical compared to type 2 diabetes remission, which depends primarily on enhanced insulin secretion.
Reducing abdominal fat mass may help reverse prediabetes
To determine the cause of increased insulin sensitivity in responders, the researchers conducted a comparative analysis of the two groups. The responders had lost more abdominal fat compared to non-responders despite losing the same amount of body weight. Visceral abdominal fat is located directly in the abdominal cavity and surrounds the intestines. Its impact on insulin sensitivity is partially attributed to an inflammatory response in adipose tissue.
Indeed, participants who went into remission also had fewer inflammatory proteins in their blood. "Since the responders showed a reduction in abdominal fat in particular, it will be important in the future to identify the factors that promote the loss of this fat depot," says Arvid Sandforth, one of the two lead authors. Surprisingly, there were no differences between the two groups in the reduction of liver fat, which is also an important risk factor for the development of diabetes. Participants who achieved remission showed a 73 percent reduced risk of developing type 2 diabetes even two years after the end of the lifestyle intervention. They also showed reduced markers of kidney damage and better status of their blood vessels.
Currently, treatment of prediabetes consists of weight reduction and lifestyle improvement to delay the onset of type 2 diabetes - but without glucose-based targets to guide the treatment process. The DZD's new analysis fills this gap: "Based on the new data, remission should be the new therapeutic target in people with prediabetes. This has the potential to change treatment practice and minimize the complication rate for our patients," says co-first author Prof. Dr. Reiner Jumpertz-von Schwartzenberg.
According to the study, remission in prediabetes can be considered to have occurred when fasting blood glucose falls below 100 mg/dl (5.6 mmol/l), 2-hour glucose below 140 mg/dl (7.8 mmol/l), and HbA1c below 5.7 percent. The likelihood of remission increases when body weight is reduced and waist circumference decreases by at least about 4 cm in women and about 7 cm in men. Researchers state that these criteria can now be used as biomarkers.
About PLIS
The Prediabetes Lifestyle Intervention Study (PLIS) was one of the initial large-scale multicentre studies conducted at the German Center for Diabetes Research under the guidance of the Tübingen site. Follow-up studies are currently underway. The study involves nine DZD sites.
The German Center for Diabetes Research (DZD) e.V.
The DZD is one of the seven German Centers for Health Research. It brings together experts in the field of diabetes research and interlinks basic research, epidemiology and clinical application. The aim of the DZD is to make a significant contribution to the successful, tailor-made prevention, diagnosis and therapy of diabetes mellitus through a novel, integrative research approach. Members of the network are Helmholtz Munich - German Research Center for Environmental Health, the German Diabetes Center DDZ in Düsseldorf, the German Institute of Human Nutrition DIfE in Potsdam-Rehbrücke, the Institute for Diabetes Research and Metabolic Diseases of Helmholtz Munich at the Eberhard Karls University of Tübingen and the Paul Langerhans Institute Dresden of Helmholtz Munich at the Carl Gustav Carus University Hospital of the TU Dresden, as well as associated partners at the universities in Heidelberg, Cologne, Leipzig, Lübeck and Munich and other project partners. www.dzd-ev.de
Helmholtz Munich
Helmholtz Munich is a top biomedical research centre. Its mission is to develop breakthrough solutions for a healthier society in a rapidly changing world. Interdisciplinary research teams focus on environment-related diseases, especially the therapy and prevention of diabetes, obesity, allergies and chronic lung diseases. Using artificial intelligence and bioengineering, the researchers transfer their findings to patients more quickly. Helmholtz Munich has more than 2,500 employees and is based in Munich/Neuherberg. It is a member of the Helmholtz Association, the largest scientific organisation in Germany with more than 43,000 employees and 18 research centres. More about Helmholtz Munich (Helmholtz Zentrum München German Research Center for Environmental Health): www.helmholtz-munich.de
Das University Hospital Tübingen (UKT)
Founded in 1805, the University Hospital Tübingen is one of the leading centres of German university medicine. As one of the 33 university hospitals in Germany, it contributes to the successful combination of high-performance medicine, research and teaching. Well over 400,000 inpatients and outpatients from all over the world benefit from this combination of science and practice every year. The clinics, institutes and centres unite all specialists under one roof. The experts work together across disciplines and offer each patient the best possible treatment based on the latest research findings. The University Hospital Tübingen conducts research for better diagnoses, therapies and healing chances; many new treatment methods are clinically tested and applied here. In addition to diabetology, neurosciences, oncology, immunology, infection research and vascular medicine are research priorities in Tübingen. The Chair of Diabetology /Endocrinology has been the centre of interdisciplinary research over the last 25 years, especially with the participation of surgery, radiology and laboratory medicine. The University Hospital is a reliable partner in four of the six German Centres for Health Research initiated by the Federal Government. www.medizin.uni-tuebingen.de
About Reiner Jumpertz-von Schwartzenberg:
Reiner Jumpertz-von Schwartzenberg is professor for Clinical Metabolism and Obesity Research at the Faculty of Medicine, University of Tübingen. Since 2021, Jumpertz-von Schwartzenberg has been senior physician for diabetology, endocrinology and nephrology as well as head of the study centre of the Institute for Diabetes Research and Metabolic Diseases at the University Hospital Tübingen. He also leads a Helmholtz Young Investigator Group and is junior research group leader in the Cluster of Excellence "Controlling Microbes to Fight Infections" (CMFI) in Tübingen, where he investigates the mechanisms underlying the development of metabolic diseases.
The focus is on the interactions between the gut microbiome and host metabolism in the context of intestinal food absorption.
Publication:
Sandforth A, Jumpertz-von Schwartzenberg R et al. (2023): Mechanisms of weight loss-induced remission in people with prediabetes: A Post-hoc Analysis of the Randomized Controlled Multicenter Prediabetes Lifestyle Intervention Study (PLIS). Lancet Diabetes Endocrinology 2023; DOI:https://doi.org/10.1016/S2213-8587(23)00235-8.
Prof. Dr. med. Andreas Birkenfeld
Director, Department of Diabetology, Endocrinology, Nephrology,
University Hospital Tübingen
Tel.: +49 (0)7071-2982735
E-Mail: andreas.birkenfeld @
@ med.uni-tuebingen.
med.uni-tuebingen. de
de
Dr. Astrid Glaser
Managing Director DZD
Tel: 089-31871619
glaser@dzd-ev.de
University Hospital Tübingen
Communication and Media Office
Hoppe-Seyler-Straße 6, 72076 Tübingen
Tel. 07071 29-88548
Related Articles



The Conversation